|
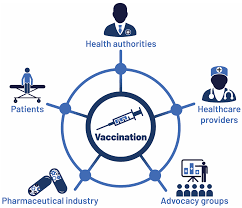
| Photo from mayoclinic.org |
The uterus is a hollow pear-shaped organ placed in a woman’s pelvis between the bladder and the rectum. The uterus is also known as the womb. It is the place where a baby develops when a woman is pregnant. The uterus is divided into three sections:
- The cervix: the small bottom portion of the uterus.
- The isthmus: the large region at the center.
- The fundus: the dome-shaped top part.
The uterus is divided into three layers: the endometrium (inner layer), the myometrium (the thickest layer, almost completely formed of muscle), and the serosa (the thin outer lining of the uterus).
During a woman’s childbearing years, her ovaries normally release an egg every month, and the endometrium thickens and develops in preparation for pregnancy. If the woman is unable to conceive, the endometrial lining exits her body through her vagina, a process known as menstruation. This process continues until a woman’s ovaries stop producing eggs, at which point she enters menopause.
UTERINE CANCER
Uterine cancer is the most prevalent type of cancer that affects a woman’s reproductive system. Uterine cancer develops when healthy cells in the uterus alter and expand uncontrollably, generating a mass known as a tumor. A tumor might be malignant(cancerous) or benign ( non – cancerous). A malignant tumor is one that can grow and spread to other regions of the body. A benign tumor can grow but will not spread to other parts of the body.
Noncancerous uterine disorders include:
- Fibroids: Tumors in the uterine muscle that are benign.
- Benign polyps: Abnormal growths in the uterine lining.
- Endometriosis: Endometrial hyperplasia is a disorder in which endometrial tissue, which normally lines the interior of the uterus, is discovered on the outside of the uterus or other organs.
- Endometrial hyperplasia: A condition in which the uterine lining has an increased number of cells and glandular structures. Endometrial hyperplasia can comprise normal or abnormal cells, as well as simple or complicated glandular structures. Endometrial hyperplasia with abnormal cells and complicated glands increases the risk of getting cancer in the uterine lining.
Uterine cancer is classified into two types:
Adenocarcinoma: This kind accounts for more than 80% of all uterine malignancies. It is formed by cells in the endometrium. Endometrial cancer is the most prevalent name for this type of cancer. Endometrioid carcinoma is a frequent subtype of endometrial cancer. Treatment for this type of cancer varies based on the tumor’s grade, how deep it spreads into the uterus, and the disease’s stage or extent. Serous, clear cell, and carcinosarcoma are less prevalent subtypes of uterine adenocarcinoma. Carcinosarcoma is a cancer that combines adenocarcinoma and sarcoma.
Sarcoma: This type of uterine cancer occurs in the uterine glands’ supporting tissues or the myometrium, which is the uterine muscle. Sarcoma contributes for roughly 2% to 4% of all uterine cancers. Endometrial sarcoma has several subtypes, including leiomyosarcoma, endometrial stromal sarcoma, and undifferentiated sarcoma.
Cancer of the uterine cervix is treated differently than cancer of the uterus.
UTERINE CANCER: GENETICS AND FAMILY HISTORY
A increased risk of uterine cancer can be inherited, which means it can be passed down from generation to generation or may miss a generation to appear in the next. This happens around 5% of the time. Lynch syndrome is the most usually connected with inherited uterine cancer. Lynch syndrome is also linked to a variety of other cancers, including colon, kidney, bladder, and ovarian cancers.
DNA mistakes can occur when cells divide and multiply. The body contains six proteins that correct these mistakes. If one of these proteins fails to function properly, mistakes in the DNA can accumulate and cause enough DNA damage for cancer to grow. This issue with DNA repair is known as a mismatch repair defect (dMMR). dMMR is the most common symptom of Lynch syndrome.
Lynch syndrome can be detected in cancer using a particular staining technique known as immunohistochemistry (IHC). The majority of Lynch syndrome cases are caused by defects in one of four DNA repair proteins. IHC only tests these four proteins on a regular basis. If IHC reveals that your cancer lacks one of these DNA repair proteins, or if you have a family history of cancer linked to Lynch syndrome, consult your doctor and/or a genetic counselor. However, IHC is only a screening test, and additional genetic tests are required to confirm a Lynch syndrome diagnosis. Lynch syndrome does not affect everyone who has a tumor that lacks one or more of these DNA repair proteins. The modifications could potentially be the result of a process known as DNA methylation, which normally silences one of the tumor’s more common dMMR genes.
Family members may also wish to be tested. People who have Lynch syndrome should tell their doctors so that they can be screened more frequently for Lynch-associated cancers, such as colonoscopies. Other family members may choose to consider uterine and ovarian cancer prevention surgery.
If you have uterine cancer, check with your doctor to see if it may be tested for Lynch syndrome and other genetic disorders.
SYMPTOMS AND SIGNS OF UTERINE CANCER
The following symptoms or indicators may be experienced by women with uterine cancer. Women with uterine cancer may not have any of these alterations at all. Alternatively, the origin of a symptom could be a medical disease other than cancer.
- Vaginal bleeding, spotting, or discharge that is unusual. This includes menorrhagia, which is excessively heavy or protracted bleeding, and/or abnormal uterine bleeding in premenopausal women (AUB).
- A Pap test yielded abnormal results.
- Pain in the lower abdomen.
The most prevalent symptom of endometrial cancer is abnormal vaginal bleeding, which can range from a watery, blood-streaked flow to a more bloody flow. Vaginal bleeding during or after menopause is frequently an indication of a problem.
STAGES AND GRADES OF UTERINE CANCER
Staging describes where the cancer is present, whether or not it has spread, and whether or not it is impacting other sections of the body.
Doctors utilize diagnostic tests to determine the stage of cancer, and they may require information based on tissue samples obtained after surgery. As a result, staging may not be complete until all tests have been completed and the tumor has been removed surgically. Knowing the stage assists the doctor in determining the best course of therapy and can help estimate a woman’s prognosis, or possibility of recovery. Distinct forms of cancer have different stage descriptions. The International Federation of Obstetrics and Gynecology (FIGO) staging system is used for uterine cancer.
FIGO stages for uterine adenocarcinomas
The stage gives a consistent language for specialists to describe the cancer, allowing them to collaborate to determine the best treatments. The FIGO method is used by doctors to determine the stage of endometrial cancer.
Stage I: The cancer has only been discovered in the uterus or womb and has not progressed to other parts of the body.
- Stage IA: The cancer is only identified in the endometrium or in less than half of the myometrium.
- Stage IB: The tumor has progressed to at least half of the myometrium.
Stage II: The tumor has spread from the uterus to the cervical stroma but has not progressed to the rest of the body.
Stage III: The cancer has gone beyond the uterus but is still confined to the pelvic region.
- Stage IIIA: The cancer has spread to the uterine serosa and/or fallopian tube and ovarian tissue but not to other regions of the body.
- Stage IIIB: The tumor has progressed to the vaginal or uterine cavity.
- Stage IIIC1: The cancer has spread to the pelvic lymph nodes in the region. Lymph nodes are small, bean-shaped organs that aid in the fight against infection.
- Stage IIIC2: The cancer has spread to the para-aortic lymph nodes and may have migrated to the regional pelvic lymph nodes as well.
Stage IV: The cancer has spread to the rectum, bladder, and/or other organs.
- Stage IVA: The cancer has progressed to the rectum or bladder mucosa.
- Stage IVB: The cancer has spread to the groin lymph nodes and/or to distant organs such as the bones or lungs.
Grade (G)
Doctors also classify this sort of cancer based on its grade (G). When examined through a microscope, the grade describes how closely cancer cells resemble healthy cells.
The cancerous tissue is compared to healthy tissue by the doctor. In healthy tissue, numerous different types of cells are clustered together. If the cancer resembles healthy tissue and contains distinct cell groupings, it is referred to as “differentiated” or a “low-grade tumor.” When cancerous tissue differs significantly from healthy tissue, it is referred to as “poorly differentiated” or a “high-grade tumor.” The grade of the cancer may help the doctor forecast how rapidly it may spread. The slower the spread, in general, the better the outlook.
The letter “G” is used to denote a uterine cancer grade.
GX: The grade cannot be evaluated.
G1: The cells have completed their differentiation.
G2: The cells have reached a stage of moderate differentiation.
G3: The cells have not differentiated sufficiently.
Recurrent uterine cancer
Cancer that recurs after therapy is referred to as recurrent cancer. Uterine cancer can recur in the uterus, pelvis, lymph nodes in the abdomen, or elsewhere in the body. If there is a recurrence, it usually happens within three years of the original diagnosis, but later recurrences might happen as well.
If the disease recurs, more testing will be necessary to identify the degree of the sickness. You should discuss treatment choices with your doctor.
DIAGNOSIS OF UTERINE CANCER
Many tests are used by doctors to detect or diagnose cancer. They perform tests to see whether the cancer has spread to a different section of the body from where it began. This is referred as as metastasis. Imaging studies, such as CT scans, can reveal whether or not the cancer has spread. Images of the inside of the body are produced via imaging tests. Doctors may also conduct tests to determine which treatments are most likely to be effective.
A biopsy is the only guaranteed way for a doctor to know if a part of the body has cancer in most cases of cancer. During a biopsy, the doctor extracts a small sample of tissue for laboratory testing. If a biopsy is not possible, the doctor may recommend alternative tests to aid in the diagnosis.
Not all of the tests listed will be performed on every woman. When selecting a diagnostic test, your doctor may take the following variables into account:
- The type of cancer that is suspected.
- Your symptoms and signs.
- Your age, as well as your overall health.
- The outcomes of prior medical tests
The following tests, in addition to a physical examination, may be used to identify uterine cancer:
- Pelvic examination: The doctor examines the uterus, vagina, ovaries, and rectum for any abnormalities. A Pap test, which is frequently combined with a pelvic examination, is primarily used to screen for cervical cancer. A Pap test may occasionally reveal abnormal glandular cells caused by uterine cancer.
- Transvaginal ultrasound: An ultrasound creates a picture of interior organs by using sound waves. An ultrasound wand is placed into the vagina and pointed at the uterus to take photographs during a transvaginal ultrasound. If the endometrium appears to be overly thick, the doctor may decide to do a biopsy.
- Computed tomography (CT) scan: A CT scan uses x-rays captured from various angles to create images of the inside of the body. A computer combines these images to create a detailed, three-dimensional image that identifies any anomalies or tumors. A CT scan can be performed to determine the size of the tumor. To improve image detail, a specific dye known as a contrast medium is sometimes administered before to the scan. This dye can be injected into a patient’s vein or given to them in the form of a pill or liquid to consume.
- Endometrial biopsy: A biopsy is the removal of a small sample of tissue for microscopic examination. Other tests can indicate the presence of cancer, but only a biopsy can provide a definitive diagnosis. The sample is examined by a pathologist. A pathologist is a clinician who specializes in interpreting laboratory tests and analyzing cell and tissue samples in order to identify disease.
The doctor uses a very tiny tube to extract a little sample of tissue for an endometrial biopsy. The tube is introduced through the cervix into the uterus, and the tissue is suctioned out. This procedure only takes a few minutes.Following that, the lady may experience cramping and vaginal bleeding. These symptoms should pass quickly and can be alleviated by taking a nonsteroidal anti-inflammatory medicine (NSAID) as prescribed by your doctor. Endometrial biopsy is frequently a highly reliable method of detecting uterine cancer. Even if no abnormal cells are identified during the biopsy, people who have abnormal vaginal bleeding prior to the test may still require a dilation and curettage.
- Molecular testing of the tumor: Your doctor may advise you to undertake laboratory testing on a tumor sample to discover specific genes, proteins, and other tumor-specific components. The results of these tests can help you decide on a treatment plan.
- Dilation and curettage (D&C): A D&C is a technique that is used to extract tissue samples from the uterus. During the surgery, a woman is given anesthetic to prevent her from feeling discomfort. A D&C is frequently performed in conjunction with a hysteroscopy so that the doctor can inspect the uterine lining during the surgery. During a hysteroscopy, the doctor inserts a thin, flexible tube with a light into the vagina and uterus through the cervix. Following the removal of endometrial tissue during a biopsy or D&C, the sample is examined by a pathologist for cancer cells, endometrial hyperplasia, and other disorders.
- Magnetic resonance imaging (MRI): An MRI produces detailed images of the body by using magnetic fields rather than x-rays. The tumor’s size can be determined via an MRI. To provide a clearer image, a specific dye called a contrast medium can be administered intravenously or orally before the scan, as with a CT scan. If the treatment plan includes hormone regulation, an MRI is particularly useful for obtaining comprehensive pictures. In women with low-grade uterine cancer, an MRI is frequently used to determine how far the cancer has spread into the uterine wall. Knowing this can aid in determining whether or not a woman’s fertility can be preserved.
After the diagnostic tests are completed, your doctor will go through the results with you. If cancer is found to be the cause, more testing will be undertaken to determine how far the disease has progressed. This aids in categorizing the condition by stage and grade, as well as directing the type of treatment required.
TREATMENT OF UTERINE CANCER
In cancer care, several types of specialists, referred to as a multidisciplinary team, frequently collaborate to develop a patient’s overall treatment strategy. A gynecologic oncologist, which is a doctor who specializes in cancers of the female reproductive system, should be on your medical team. Cancer care teams comprise a number of different health care professionals, in addition to physicians, such as physician assistants, nurse practitioners, oncology nurses, social workers, pharmacists, counselors, nutritionists, and others.
The following are descriptions of the most prevalent types of uterine cancer therapies. Your treatment plan will also include treatment for symptoms and side effects, which is an important aspect of cancer care.
Treatment options and recommendations are influenced by a variety of criteria, including the kind and stage of cancer, potential side effects, overall health, age, and personal preferences. This includes whether or whether the treatment will impair your ability to have children, which is referred to as fertility. Uterine cancer is treated with one or more procedures, including surgery, radiation therapy, and systemic medicines. Combinations of these cancer treatments are frequently prescribed, however their effectiveness is determined by the stage and features of the tumor.
Take the time to read about all of your treatment options, and don’t be afraid to ask clarifying questions. Discuss the aims of each treatment with your doctor, as well as what you can expect during treatment. These discussions are known as “shared decision making.” When you and your doctors collaborate to choose therapies that meet the goals of your care, this is referred to as shared decision making. Because there are various treatment choices for uterine cancer, shared decision making is very crucial.
Concerns about sexual health and the possibility of having children
Women suffering from uterine cancer may be concerned about how their cancer treatment will effect their sexual health and fertility. Before beginning treatment, these topics should be reviewed with the health care team. Premenopausal women who are still fertile and want to protect their fertility should see their oncologist and/or a reproductive endocrinologist (REI), often known as a fertility expert, before beginning therapy. During these discussions, inquire about the fertility preservation options offered by your health insurance.
Surgery
During a surgery, the tumor and some surrounding healthy tissue, known as a margin, are removed. It is usually the initial line of defense against uterine cancer. A surgical gynecologic oncologist is a doctor who specializes in the surgical treatment of gynecologic cancer. Before undergoing surgery, consult with your health care team about the potential adverse effects of the procedure.
The following are some of the most common uterine cancer surgery procedures:
- Hysterectomy: Depending on the degree of the cancer, the surgeon will either conduct a simple hysterectomy (removal of the uterus and cervix) or a radical hysterectomy (removal of the uterus, cervix, the upper part of the vagina, and nearby tissues). For menopausal patients, the surgeon would often conduct a bilateral salpingo-oophorectomy, which is the removal of both fallopian tubes and ovaries.
A hysterectomy can be performed through abdominal incision, laparoscopy or robotically (with numerous small incisions), or vaginally. A hysterectomy is typically performed by a gynecologic surgeon, who is a surgeon that specializes in female reproductive system surgery. A camera and tools are inserted through small, keyhole-sized incisions in robotic-assisted surgery. The robotic devices are guided by the surgeon to remove the uterus, cervix, and surrounding tissue. Additional therapy may not be required if a woman has no cancer left in the tissue removed during a hysterectomy. However, regular screening and testing to check for cancer recurrence is advised.
- Lymph node removal: The surgeon may remove lymph nodes near the tumor at the same time as the hysterectomy to assess if the cancer has spread beyond the uterus. This can be accomplished with a procedure known as a sentinel lymph node biopsy or lymphadenectomy. A sentinel lymph node biopsy may entail injecting dye into the uterus during the hysterectomy and removing the few lymph nodes where the dye accumulates. In uterine cancer, this surgery has become more common than lymphadenectomy. A lymphadenectomy, also known as lymph node dissection, is a surgical surgery that removes a group of lymph nodes.
Discuss with your doctor the risks and benefits of the various surgical techniques, as well as which approach may be ideal for you.
Surgical side effects
The most common short-term side effects of surgery include pain and weariness. If a woman is in pain, her doctor will prescribe drugs to help her feel better. Other acute adverse effects include nausea, vomiting, and problems emptying the bladder and having bowel motions. A woman’s diet may be restricted to liquids following surgery, followed by a gradual resumption to solid foods.
When the ovaries are removed, the body’s synthesis of sex hormones ceases, resulting in early menopause (if the woman has not already gone through menopause). While removing the ovaries significantly limits the amount of sex hormones produced by the body, the adrenal glands and adipose tissues will still provide some hormones. A woman is likely to suffer menopausal symptoms, such as hot flashes and vaginal dryness, soon after having her ovaries removed. Discuss with your doctor how to alleviate and manage these menopausal symptoms.
Some women may experience swelling in their legs after having a lymphadenectomy, which is known as lymphedema.
A woman cannot become pregnant after having a hysterectomy. As a result, premenopausal women who want to protect their fertility and have children in the future should consult with their doctor about all of their options before beginning any medication. Fertility preservation is sometimes possible and may require less invasive surgery followed by hormone medication. Your doctor can discuss the potential risks and benefits of this method with you and provide information to assist you in making an informed decision.
Women are urged to discuss sexual and emotional side effects with their doctors prior to any uterine cancer surgery, as well as options to address these difficulties before and after cancer treatment.
The therapy choices for endometrial cancer following surgery are determined on the cancer’s stage and grade. Additional therapy may be avoided for women who have had surgery and have grade 1 or 2 cancer that has not spread to the myometrium or has spread more than halfway through the myometrium.
When contemplating your post-surgery therapy options, consult with your doctor about how each treatment may effect you. It is critical to balance the benefits of treatment in terms of perhaps preventing cancer recurrence with the hazards of treatment. Treatment hazards may include short- and long-term adverse effects, as well as a significant deterioration in your quality of life. What you consider a decline in quality of life is entirely subjective. This is why it is critical to discuss any side effects with your doctor, as well as how long they will persist and how they will affect you now and in the future.
Radiation therapy
The use of high-energy x-rays or other particles to eliminate cancer cells is known as radiation therapy. A radiation oncologist is a doctor who specializes in the use of radiation therapy to treat cancer. A radiation therapy regimen, or schedule, typically consists of a predetermined number of treatments administered over a predetermined time period. Radiation therapy can be administered both externally and inside. External-beam radiation therapy employs the utilization of a machine located outside the body to administer radiation to the pelvic region or another location specified by your radiation oncologist. Internal radiation can also be administered. Brachytherapy is a type of radiation therapy. External-beam radiation therapy may be administered alone or in conjunction with brachytherapy. Brachytherapy alone may be appropriate for some patients. External-beam radiation therapy is the most prevalent method of radiation treatment.
Some uterine cancer patients require surgery as well as radiation therapy. Radiation therapy is typically used following surgery to kill any leftover cancer cells. Radiation therapy is sometimes used prior to surgery to shrink the tumor. If a woman is unable to have surgery, her doctor may suggest radiation therapy instead.
Radiation therapy directed at the entire pelvis and/or delivered solely to the vaginal canal, known as vaginal brachytherapy, are two options for treating uterine cancer. If a woman has a grade 1 or 2 cancer that has gone through half or more of her myometrium, or a grade 3 cancer that has spread through less than half of her myometrium, she may be able to have vaginal brachytherapy instead of pelvic radiation.
Radiation therapy to the pelvis may be the best option for some women to help prevent cancer recurrence. These women have cancer that has spread through half or more of the myometrium, cancer of any grade that has spread to tissue in the cervix, or cancer that has spread outside the uterus to surrounding tissue or organs. In some cases, a woman may require only radiation therapy following surgery, only chemotherapy, or a combination of the two. Your doctor will be able to advise you on which of these solutions is best for you.
Depending on circumstances such as age and whether the cancer has spread to blood or lymphatic vessels, radiation therapy to the pelvis may also be considered for some women with grade 1 or 2 cancer that has advanced through half or more of the thickness of the myometrium.
Radiation therapy researchers are constantly seeking for new ways to improve it in order to reduce adverse effects and increase effectiveness. MRI-guided radiation therapy is one option being investigated. An MRI scan is paired with a linear accelerator, which is a machine that administers radiation therapy, during this procedure. The MRI gives real-time images of the area being treated with radiation therapy, allowing for more accurate and precise radiation therapy delivery. This reduces the quantity of healthy tissue exposed to radiation while focusing treatment on the tumor and afflicted organs. The US Food and Drug Administration has currently approved one system for MRI-guided radiation therapy (FDA). Other approaches to MRI-guided radiation therapy are being investigated.
Radiation therapy side effects may include weariness, moderate skin responses, upset stomach, and loose bowel movements, depending on the quantity of radiation therapy administered. The majority of negative effects disappear shortly after therapy is completed, however long-term side effects are possible. Discuss what you can expect and how side effects will be addressed with your radiation oncologist.
Chemotherapy
Chemotherapy is the use of medications to eradicate cancer cells, typically by preventing the cancer cells from growing, dividing, and proliferating. Chemotherapy is generally used following surgery for endometrial cancer. If the endometrial cancer returns after the person’s initial treatment, chemotherapy is also recommended.
A chemotherapy regimen, or schedule, typically consists of a predetermined number of cycles administered over a predetermined time period. A patient may be administered one medicine at a time or a mixture of drugs at the same time.
Chemotherapy’s purpose is to either eradicate any cancer that remains after surgery or to reduce the disease and slow its growth if it returns or has spread to other places of the body. Although chemotherapy can be administered orally, the majority of medications used to treat uterine cancer are administered intravenously. IV chemotherapy is administered either directly into a vein or via a catheter, which is a thin tube placed into a vein.
Chemotherapy side effects vary depending on the individual, the type of chemotherapy used, and the amount, but they can include fatigue, infection risk, nausea and vomiting, hair loss, loss of appetite, and diarrhea. These adverse effects normally fade away once the treatment is completed. Over the last decade, advances in chemotherapy have included the introduction of novel medications for the prevention and treatment of side effects, including as antiemetics for nausea and vomiting and growth factors to avoid low white blood cell counts and lower the risk of infection.
Other potential adverse effects of uterine cancer chemotherapy include inability to conceive in the future and having early menopause if the patient has not already undergone a hysterectomy. If you want to keep your fertility, consult with your doctor before beginning therapy. Some medicines, on rare occasions, cause hearing loss. Others may harm the kidneys. To protect their kidneys, patients may be given extra fluid intravenously. Discuss with your doctor the potential side effects of chemotherapy and how they can be avoided or managed.
Hormone therapy
Hormone therapy is used to slow the growth of specific types of uterine cancer cells with hormone receptors. These tumors are typically adenocarcinomas with a grading of 1 or 2.
Hormone therapy for uterine cancer frequently entails taking a high dose of the sex hormone progesterone in pill form. Hormone-expressing intrauterine devices (IUDs) and aromatase inhibitors (AIs) such as anastrozole (Arimidex), letrozole (Femara), and exemestane (Aromasin) are also commonly used in the treatment of breast cancer. An AI is a medication that decreases the quantity of estrogen in a woman’s body by preventing tissues and organs other than the ovaries from making it. Hormone therapy may also be utilized in women who are unable to undergo surgery or radiation therapy, or it may be used in conjunction with other methods of treatment.
Fluid retention, increased hunger, sleeplessness, muscular aches, and weight gain are all possible side effects of hormone therapy. The majority of side effects are controllable with the assistance of your health care team. Consult your doctor about what to expect.
Targeted therapy
Targeted therapy is a type of cancer treatment that targets specific genes, proteins, or the tissue environment that contributes to cancer growth and survival. This method of treatment inhibits cancer cell growth and spread while limiting damage to healthy cells.
The targets of all cancers are not the same. Your doctor may order tests to determine the genes, proteins, and other variables in your tumor in order to find the most effective treatment. This enables clinicians to provide the most effective treatment to each patient whenever possible. Furthermore, research studies are continuing to learn more about specific molecular targets and new treatments aimed at them.
Uterine cancer targeted therapy is offered in clinical trials and, in some cases, as part of standard-of-care treatment regimens. Uterine cancer targeted therapy comprises the following treatments:
- Anti-angiogenesis therapy: Anti-angiogenesis therapy aims to halt angiogenesis, or the process of forming new blood vessels. Because tumors require the nutrients given by blood vessels to develop and spread, anti-angiogenesis medicines aim to “starve” the tumor. Bevacizumab (Avastin) is an anti-angiogenesis medication that is used to treat uterine cancer.
- Mammalian target of rapamycin (mTOR) inhibitors: Mutations in the mTOR pathway are frequently detected in endometrial cancer. People with advanced or recurring uterine cancer may be treated with everolimus, a medication that blocks this pathway (Afinitor). Ridaforolimus and temsirolimus (Torisel), a targeted medication licensed to treat a kind of kidney cancer termed renal cell carcinoma, are two more drugs being researched that target this pathway.
- Targeted therapy to treat a rare type of uterine cancer: Uterine serous carcinoma is an uncommon but deadly form of endometrial cancer. The HER2 gene is expressed in approximately 30% of these cancers. Researchers discovered that trastuzumab (Herceptin) paired with a mixture of chemotherapy was beneficial in treating certain types of cancers in a phase II clinical trial. Trastuzumab is a HER2-targeted treatment that is primarily used to treat HER2-positive breast cancer.
The side effects of various targeted therapy vary. Consult your doctor about these potential side effects and how to manage them.
Immunotherapy
Immunotherapy, also known as biologic therapy, is intended to increase the body’s natural defenses against cancer. It employs components created by the body or in a laboratory to enhance, target, or restore immune system activity.
Immunotherapy is more effective in uterine tumors with mismatch repair abnormalities. Pembrolizumab (Keytruda), an immunotherapy medicine, is approved to treat malignancies with high microsatellite instability (MSI-high) or dMMR, regardless of where the tumor is located in the body. If no other treatments have worked, pembrolizumab can be used to treat uterine cancers with dMMR.
To treat advanced endometrial cancer, a combination of lenvatinib (Lenvima), a targeted therapy medication, plus pembrolizumab is also approved. This combination can be used to treat disease that isn’t MSI-high or dMMR, hasn’t responded to systemic therapy, and can’t be cured with surgery or radiation therapy. Lenvatinib has been linked to an increase in blood pressure.
The FDA approved the immunotherapy medication dostarlimab (Jemperli) in April 2021 to treat recurrent or advanced endometrial cancer with dMMR that has progressed during or after platinum-containing chemotherapy. Dostarlimab is administered intravenously every three weeks. Fatigue, nausea, diarrhea, and constipation are the most prevalent adverse effects.
Different forms of immunotherapy might result in a variety of adverse effects. Skin rashes, flu-like symptoms, diarrhea, and weight fluctuations are all common adverse effects. Consult your doctor about the potential adverse effects of the immunotherapy that has been prescribed for you.
Metastatic urine cancer
Doctors refer to cancer that has spread to a different place of the body from where it began as metastatic cancer. If this occurs, it is advisable to consult with specialists who have treated similar cases in the past. Different doctors may have differing views on the optimal conventional treatment strategy. Clinical trials are another possibility.
Radiation therapy or surgery may be part of your treatment plan, particularly if you have recurrent pelvic cancer. Cancer that has progressed to other places of the body may benefit from hormone therapy. Chemotherapy is used to treat cancers that are advanced or do not respond to hormone therapy. Standard-of-care therapy options for women with stage IV uterine cancer are numerous. They are also urged to think about taking part in clinical trials. Palliative treatment will be necessary to alleviate symptoms and side effects.
A diagnosis of metastatic cancer is extremely stressful and challenging for the majority of people. You and your family are encouraged to express your feelings to doctors, nurses, social workers, and other members of the health care team. It may be beneficial to speak with other sufferers, such as through a support group.
Remission and the possibility of recurrence
When cancer cannot be identified in the body and there are no symptoms, the patient is said to be in remission. This is often known as having “no evidence of illness,” or NED.
Remission can be either temporary or permanent. Many people are concerned that the cancer will recur as a result of this uncertainty. While many remissions are durable, it is vital to discuss the potential of the cancer returning with your doctor. Understanding your recurrence risk and treatment options may make you feel more prepared if the cancer returns. One of the primary goals of follow-up care is to monitor for recurrence and to manage any late effects or long-term side effects of treatment.
Recurrent cancer occurs when the cancer returns after the initial treatment. It may return in the same location (called a local recurrence), nearby (called a regional recurrence), or elsewhere (distant recurrence). Some recurrent cancer symptoms are similar to those experienced when the disease was originally diagnosed:
- Bleeding or discharge from the vagina
- Pelvic, abdominal, or back of the legs pain
- Having difficulty or experiencing pain when urinating
- Loss of weight
- Coughing/shortness of breath that persists
When a recurrence happens, a fresh round of testing will begin to learn everything we can about it. Following the completion of this testing, you and your doctor will discuss treatment choices. The treatments outlined above, such as hormone therapy, radiation therapy, and chemotherapy, are frequently included in the treatment plan, but they may be administered in a different mix or given at a different pace. When a cancer recurrence is tiny or restricted, called a localized recurrence, surgery may be recommended. Your doctor may recommend that you participate in clinical studies that are looking for new ways to treat this sort of recurring cancer. Palliative care will be essential for reducing symptoms and side effects regardless of the treatment plan you choose.
People suffering from recurring cancer frequently experience emotions such as bewilderment or anxiety. You are urged to discuss these feelings with your health care provider and inquire about support options to assist you in coping.